 They compared the 50 who got DD after the initial three shocks, to the 229 who were treated with repeated single biphasic defibrillations and found no difference in neurologically intact survival, ROSC, survival to hospital admission, or survival to hospital discharge. 3-5,7-9 Nevertheless, a recent retrospective study of 279 OHCAs who had RVF after three 200J single biphasic defibrillations did not find a benefit. Several case reports and small case series have been published on DD for OHCA, with reports of ROSC as high as 57.1% and neurologically intact survival to discharge as high as 28.6%. 3Īlthough DD has long been a procedure employed by electrophysiologists to cardiovert iatrogenic RVF in the electrophysiology lab, use of this technique for out-of-hospital cardiac arrest (OHCA) with RVF is a relatively new concept. Proposed theories as to why DD may be efficacious include the delivery of more energy to overcome the defibrillation threshold as well as the addition of another defibrillation vector which may overcome poor pad placement or thoracic impedance from, for instance, pulmonary edema or hyper-inflated lungs. 2-5 Both defibrillators are charged to either 200J or maximum energy, and the patient is shocked simultaneously from both defibrillators. However, two sets of defibrillator pads are usually placed in the anterior-lateral and anterior-posterior positions. There is great variation in the way DD is performed. RVF is generally defined as 3 or more episodes of sustained or recurrent VF despite appropriate defibrillation attempts. The patient is then transferred to the catheterization lab where a 100% occlusion of the right coronary artery is found and stented.ĭD, also known as double sequential defibrillation, double sequence defibrillation, dual simultaneous defibrillation, or dual axis defibrillation, refers to the use of two defibrillators to electrically cardiovert a patient in refractory VF (RVF). An electrocardiogram reveals atrial fibrillation with evidence of ST-elevation myocardial infarction. The patient achieves return of spontaneous circulation (ROSC) after 45 minutes of downtime. 
An additional defibrillator is acquired, with plans to perform dual defibrillation (DD).Īn additional anterior-posterior set of defibrillation pads are added to the traditional anterior-lateral set (Figure 1), and he is shocked near-simultaneously from both pads at 200J. After another single biphasic defibrillation, he is given lidocaine, magnesium, calcium gluconate, and sodium bicarbonate. 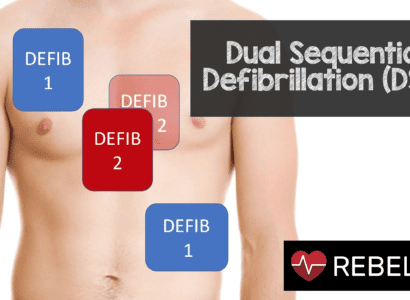
Upon arrival to the emergency department (ED), the patient remains in VF. They deliver seven single biphasic defibrillations, two doses of amiodarone, and one dose of epinephrine per Advanced Cardiac Life Support (ACLS) recommendations. 
When EMS arrives, they find the patient in ventricular fibrillation (VF). Proposed theories as to why DD may be efficacious include the delivery of more energy to overcome the defibrillation threshold as well as the addition of another defibrillation vector.Ī 44-year-old male with no past medical history collapses at home in front of his son, who calls 911 and begins CPR. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
